Dr. Elke Loeffler

The European Network for Public Administration (ENPA) is a newly founded independent learned society led by public administration academics for the theoretical and practical improvement of public administration.
I attended its inaugural conference, held at the top University ASE in Bucharest, in my role as co-founding Board Member and co-chair of the ENPA Research Group on Public Participation and Co-Production. There was also a strong representation of UKAPA – the UK Association for Public Administration. This event showcased a number of innovative formats, including a plenary in interview format on democratic resilience and a highly interactive ‘collaborative discussion’ session on systems resilience, as well as providing a highly-valued Conference Buddy Scheme for Doctoral Researchers.
During the conference it became clear that resilience is now a major emerging theme in public management research and practice. For many local councils this concept has so far been mainly used in relation to emergency response and planning. However, the LGA in the UK considers this to be a ‘whole council effort’, going beyond small emergency teams.
Moreover, the discussions at the ENPA Conference revealed that resilience is not just about sudden, extreme emergencies but about creeping crises such as democratic backsliding and and prolonged failures such as delayed access to public healthcare. While robust governance (Ansell, Torfing and Trondal, 2025, Robust Public Governance in a Turbulent Era) – the ability of a system to maintain its operations despite disruption – is important, resilience is more demanding – it is about the capacity for adaptation in the service system to recover to the same or high outcomes after a disturbance – or as a former UK Prime Minister expressed it “building back better”.
The keynote speakers also discussed the need for public administration scholars to strengthen resilience. Don Moynihan from the University of Michigan highlighted that rule-bound public administration and independent academic research often become targets for populist leaders. He suggested that, in times of democratic backsliding, delivering evidence-based descriptions of current situations and contexts may be more effective than sophisticated, time-consuming causal analysis. While not as analytically powerful, making it clear what is actually happening may make a greater impact on public attitudes, and eventually on public policies, than complex modelling. This argument gave rise to considerable debate in the coffee breaks!
The collaborative session in our Research Group demonstrated that local government resilience is not enough – we also need resilient communities, service users and markets. This brings in the potential role of user and community co-production in strengthening systems resilience. For example, Jan Dumkow from the Helmut Schmidt University Hamburg provided a current action-research project involving co-design of an app for and with people with learning disabilities so that service providers would be able to provide tailored information in the case of emergencies.
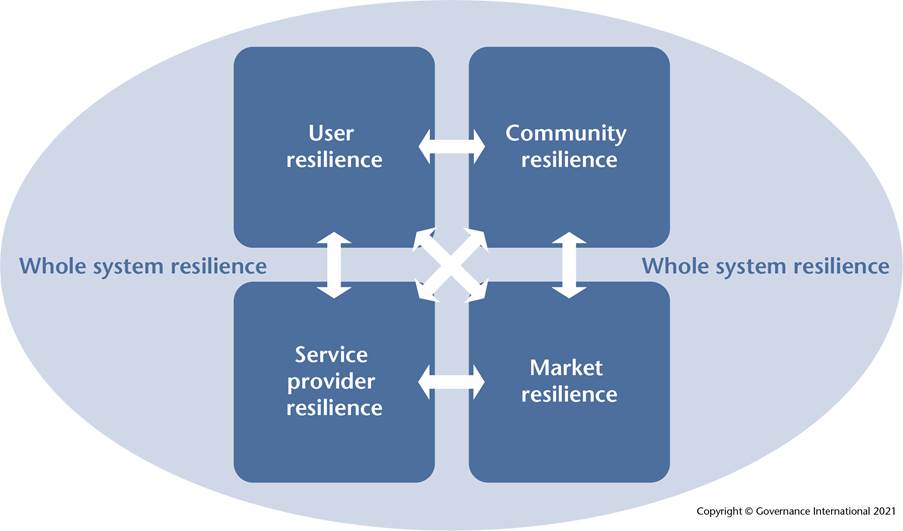
The ‘whole systems resilience network’ depends on each element in the network of user-community-provider-market resilience being sound and well-balanced with the other elements (Bovaird and Loeffler 2024). The resilience network constitutes a dynamic system, in which each of the stakeholder groups is always looking to learn and to improve, with the consequence that a weak link in the network reduces the overall capability of the system. However, a systematic literature review which I undertook with Sanneke Kuipers (Leiden University) and Marie-Christine Therrien (Ecole Nationale D’Administration Publique, Montreal), on the role of co-production in strengthening resilience in extreme crisis, revealed that user and community involvement is largely absent in current evaluations of crisis interventions. This is cause for concern and highlights the urgent need for more engaged research with local communities and local councils on how to strengthen all links in the whole systems resilience network. INLOGOV is well situated to work with local councils and communities on this issue, given its expertise on co-production and social prescribing.

Dr. Elke Loeffler is an Associate of INLOGOV and Director of Governance International. She undertakes applied research on local public services and has research interests in community co-production and resilience. Elke is Board Member of the European Network of Public Administration, Vice-Chair for Doctoral Research in UKAPA and Chair of the Public & Nonprofit Management Group at EURAM.




